 Region 3 of Kentucky’s Medicaid system, comprising Jefferson and nearby counties, is in the throes of a major reorganization. Beginning January 1, the previous monopoly to provide Medicaid services held by a consortium of providers organized by the University of Louisville was withdrawn. State contracts were offered to three additional Medicaid Managed Care Organizations (MCOs). The timing of this major change was not the most felicitous, given that the statewide Medicaid managed care system newly put in place January 2012, could be said sympathetically to be in chaos. Medicaid managed care has been operational in Region 3 for several years and was providing acceptable clinical services, albeit under a cloud of abusive if not illegal management by its UofL-controlled financial administration. (One might say it was used as a slush fund. No one went to jail, but people lost their jobs and a major reorganization was demanded by the state.)
Region 3 of Kentucky’s Medicaid system, comprising Jefferson and nearby counties, is in the throes of a major reorganization. Beginning January 1, the previous monopoly to provide Medicaid services held by a consortium of providers organized by the University of Louisville was withdrawn. State contracts were offered to three additional Medicaid Managed Care Organizations (MCOs). The timing of this major change was not the most felicitous, given that the statewide Medicaid managed care system newly put in place January 2012, could be said sympathetically to be in chaos. Medicaid managed care has been operational in Region 3 for several years and was providing acceptable clinical services, albeit under a cloud of abusive if not illegal management by its UofL-controlled financial administration. (One might say it was used as a slush fund. No one went to jail, but people lost their jobs and a major reorganization was demanded by the state.)
Given that the new contracts and procedures in Region 3 are essentially the same as those now used statewide, it is instructive to see how things have been going in the rest of the state. Alas, the precedents are not rosy. “Medicaid-Meltdown” is a term that is frequently being used. The rocky start may be one of the reasons the state is withholding its approval of expanding the Medicaid program under the new federal Accountability and Affordability Act to provide more Kentucky individuals health insurance coverage. In that regard, an interim report funded by the Foundation for a Healthy Kentucky and prepared by the Urban Institute and the University of Kentucky is receiving much attention nationally and is relevant to Region 3’s future. (Click the “Medicaid” category link in the left column of the Blog home page for available earlier comments.)
Medicaid managed care in Kentucky is struggling.
It should be noted that the report, “Evaluation of Statewide Risk-Based Managed Care in Kentucky– A First Year Implementation Report,” is only current through mid-2012 and that one of the authors is itself a Medicaid provider. A major deficiency is that no Medicaid beneficiaries were included among the parties interviewed for the report. The initial findings are well known and probably not unexpected. A very short time was available to prepare for such a major transformation. The MCOs had difficulty establishing provider networks in areas in which they were new. Many providers refused to sign contracts, and certainly not with all three new statewide MCOs. Medical data on which payments to the plans were based were suspect. Computers talked to each other slowly if at all. There were high rates of beneficiaries switching plans making continuity difficult. Few of the required case-management or quality and utilization initiatives were available. Inexperience with managed care could be seen everywhere. Provider directories were incomplete. Major providers pulled out of the system altogether. Adversarial positions and lawsuits are blossoming. You can download the relatively brief report yourself here. It does not present a pretty picture. It is easy to place blame on the Commonwealth or the MCOs, but it is clear to me that providers were more than willing not to cooperate. It is easy to sabotage managed care. This is one of the costs to us of not having a single payer system.
Death panels or knights in shining armor?
There were many complaints about preauthorization requests for medical services and drugs being denied. That is not necessarily a bad thing. Denying medically unnecessary or wasteful expenses is why the state hired these organizations on our behalf in the first place. However, by most reports, the systems in place allowing preauthorization, communication of denials, and appeals took too long and were confusing.
Events in Region 3.
So why is all this relevant to the brand new Medicaid Managed care system in Region 3? With the exception of Passport, there were only a few months available for the three new MCOs to get their act together. While the new organizations had experience in other states and may have had the computer and other systems in place to do the job, they did not have preexisting networks of hospitals, physicians, and other providers in place. Worse, they were at the mercy of the providers of Region 3 who already had satisfactory, if not cosy, relationships with Passport. The fact that UofL provides most of the specialist care for Region 3 also gives Passport a handful of trump cards. The new Region 3 system has been operational for barely more than a month. I and others will continue to observe how things play out in Region 3. For the purposes of this article, I will focus on what is happening with respect to enrollment of beneficiaries by the four plans. I see trouble ahead.
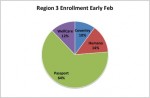
Current Enrollment in Region 3.
I asked the Kentucky Department of Medicaid Services to provide me with current enrollment numbers in the four plans. Originally, the state distributed beneficiaries more or less equally among the plans. Beneficiaries were given an option to switch from their assigned plan for a limited period last December, and for a longer period through the end of March. Switch they did indeed! As of this week, Passport has corralled 64% of all beneficiaries, nearly twice as much as the other three plans combined! It might be fairly asked if the other plans have enough beneficiaries to be clinically effective or financially viable. Given that there are still 7 weeks yet to run when beneficiaries can switch plans this year, I would expect Passport’s share to grow even larger.
I report these numbers as I received them. I confess it makes me more than a little nervous that the total number of enrollees has been exactly the same (164,608) since the original assignment. I would have thought that there would have been some change in the number of beneficiaries in the past 3 months. This highlights one of the problems facing the state and its Medicaid providers– working with current information.
How did this happen?
Although I personally regret that Kentucky (as perhaps most Medicaid programs) serves its patients in what are in my opinion second-tier systems that do not compete well for patients with other sources of payment, Passport has been providing better than acceptable medical care– even better than pre-managed care Medicaid. Passport properly from the start included a clinical (but not financial) advisory structure that was fairly broadly representative of providers. There was more buy-in by providers than in the usual managed care systems. For this and other reasons, Passport and its contracted providers grew more or less comfortable working with each other. Medicaid has become a reliable source of income for them. (I have no idea how non-participating providers feel about all this.) If I were a Medicaid beneficiary having to deal with three new plans, I would ask my doctor what to do. I think the beneficiaries are listening.
It is to Passport’s advantage that a large number of its physicians are closely aligned with the University of Louisville in whose interest Passport was largely formed in the first place. I wonder what plan these physicians might recommend? Passport had a head start and wisely and aggressively reached out to non-University and other physicians with webcasts and printed materials recommending that their patients switch to Passport. Even I received an issue of a medical newspaper sent to physicians and the public that was intended for display in waiting rooms sponsored by Passport and which emphasized switching plans. In my opinion it gave at least the initial appearance of a non-aligned public service announcement but its real goals seemed apparent to me. (Others may disagree.) It is likely that additional materials were distributed by Passport and the other MCOs.
Is the market still cornered?
The whole point of opening up the Medicaid market in Region 3 and the rest of Kentucky was to be able to provide more and better care at less cost, or more care at the same cost. Health insurers around the country are consolidating and gearing up for expansion of the Medicaid program to more individuals and families. However, is a given that without the support or at least the cooperation of physicians and other providers, Managed Care Organizations are doomed to fail. In Region 3, the three new MCOs face an uphill struggle to gain a foothold. It is likely they will need to underwrite considerable financial losses to buy the time needed show that they might provide more services or do a better job. Coventry and WellCare have statewide systems in place to help, but by most accounts are losing money already. (Passport has the luxury of not having to service the rest of the state.) Humana is new to the Kentucky Medicaid managed care market, but has much experience and local non-Medicaid networks that in a non-egalitarian world might help. None-the-less, I bet my usual Martini in your favorite Louisville bar, that one or more of the new MCOs will attempt to withdraw from Region 3 in the next two years. I hope at least one of you will take me up on this bet so we can discuss the matter and so that I can be educated from another perspective.
If you can provide the rest of us with some additional insight into how Passport was so successful in retaining its dominant role as a Medicaid Provider Organization in Louisville and Region 3, I urge you to tell us in a comment below, or communicate with me confidentially using the link in the left column.
Peter Hasselbacher, MD
President, KHPI
Emeritus professor of Medicine, UofL
February 8, 2013.
Download table with enrollment data and chart as pdf document.
Download Urban Institute Report. (Word document)

Where does all the money go?
On Feb. 6, the day before I posted this, Medicaid officials and executives from statewide managed care plans testified in Frankfort at a meeting of the House Budget Subcommittee on Human Resources. I have not yet been able to obtain minutes or handouts from the meeting but saw a report in the Ashland Independent Online.
In brief summary, Medicaid officials acknowledge a rocky start but thought that current complaints are not totally out of line when compared to private health insurance. A senior vice president for one of the statewide MCOs was less sanguine, and reiterated at least some of the criticisms we have mentioned before in these pages.
The stunning piece of information revealed was that the state is paying rates to the new Region 3 plans that are 30% higher than for Medicaid beneficiaries in the rest of the state! Since two of the statewide MCOs also service Region 3, they should know.
I have commented earlier that I have never personally seen any convincing data that Passport has saved the state (and therefore our pocketbooks) any money. It is my understanding there were not even any systems in place to make such a determination. I do not accept that Medicaid patients in Louisville are any more or less sick than those elsewhere in the state. Therefore, if indeed based on historical utilization, Louisville and Region 3 burn through 30% more money, I think we the public need a much better accounting. Given the fact that the finances of these operations have so little transparency or accountability, how can we ever know. It took an insider to reveal the statistic. Tell me it isn’t true!
If anyone out there has access to relevant information, or the documents from the committee hearing, please share them with me.