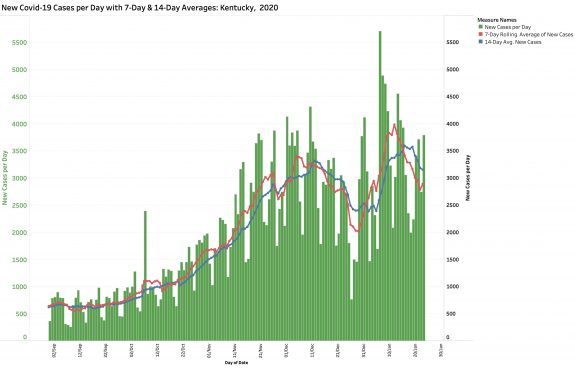
As of the end of the week on January 23d, the jagged sawtooth profile of tall daily peaks of followed by deep dips of new cases over weekends and holidays persists, but the peaks are not as high as in early January and our 7-Day and 14-Day averages are back down to about where they were in early December. The number of new cases weekly has been dropping for the past three full weeks. To the extent that Test Positivity Rates are an indicator of community epidemic spread, they remain high but have been trending downwards over the past week. These are all good signs, but we would all like to see a decrease in new cases at this time of rapid epidemic spread nationally and the emergence of new strains of the virus whose impact in the USA remains to be determined. (It will also be reassuring news to learn that the state’s broken case-reporting pathway from its testing vendors had been repaired.)
Deaths.
We cannot be fully comfortable that our Covid-19 epidemic has stabilized, even if only at a new “plateau” until deaths also begin to fall. Yesterday’s reported 49 deaths was the highest Saturday total by far, as was last week’s count of 293 (compared to the previous weekly total of 217). For a limited period of time we can understand a sustained death rate as the consequence of the epidemic surges of prior weeks, but eventually we will need to consider other explanations such as whether the virus is becoming more lethal or if there are flaws in our overall reporting systems.
Serious illness.
State-wide averages of hospital ICU, and ventilator utilization remain at high levels where they have been since early December. These patients represent the sickest of Covid-19 disease and the length-of-stay in hospitals can be long for some individuals, especially ventilator patients. It might be predicted that a fall in hospital utilization would lag the incidence of new cases, but not all hospitalizations are long. We would like to see this indication of epidemic morbidity begin to ease. A hospital-specific report might be illuminating. The federal government has begun to make such data available and I will try pull out Kentucky’s numbers.
The data and complete data visualizations underlying this summary are available on KHPI’s Tableau Public website. Those data are generally updated daily even if I do not comment on it.
Covid-19 is a big deal!
The American Cancer Society estimates that in 2021 there will be 30,270 new cases of cancer in Kentucky. As of last week, the state had 338,034 cases of Covid-19 disease in much less than a full year. There are likely to be more than ten times more Covid cases than new cancers! Seems to me there is a discrepancy in public enthusiasm to get behind public health and other medical interventions of prevention and treatments of these disorders. Could the vast public relations, fund-raising, and industry money driving our approaches to cancer be making a difference? Public health measures alone can claim a major if not the majority role in driving down our cancer incidence and deaths. These were working long before aggressive chemotherapy came along. Why not give Covid-19 and the epidemics that will surely follow the same opportunity to improve our lives?
How ’bout them vaccines?
The overall appetite for immunization in the community at present vastly outstrips the ability of the state to acquire the vaccine itself or the ability to finance and staff the widely distributed, high-throughput locations needed to give the shots throughout the Commonwealth. As of last Thursday, 250,847 initial or booster immunizations were given to individuals, with a focus on long term care residents and their care tenders, and frontline healthcare workers. Broadening eligibility for immunization to include seniors 70 and over immediately overwhelmed the system. The available vaccines are at present FDA-approved only for adults 18 and older. There are an estimated 3.47million of such in Kentucky. A back-of-the-envelope calculation tells me that for the remaining unimmunized individuals to get their first shot by the end of June, we need to be processing 21,490 people per day, 7-days a week. The two vaccines now available require a booster shot 3 weeks later. When the need for this 2d shot is included, the daily target necessary for 100% coverage will double to over 40,000. Obviously, the availably of current and potential new vaccines; and the equipment, manpower, and locations available will determine how long it takes to cover the Commonwealth.
The vaccines work.
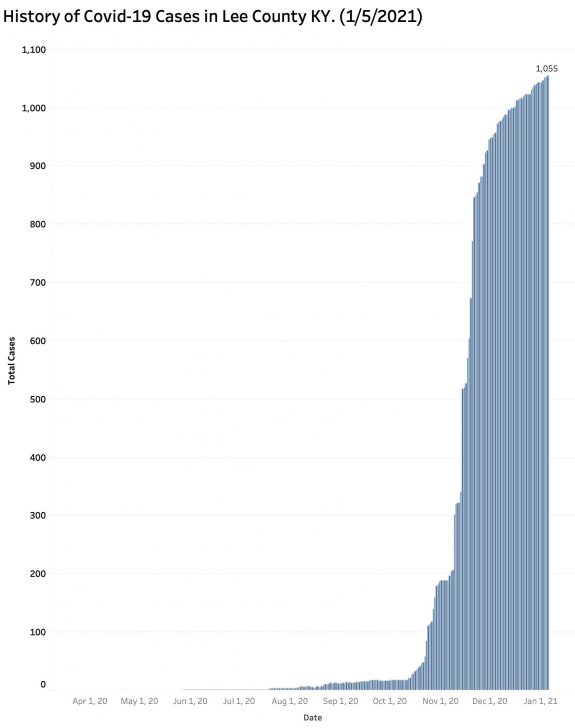
I recently summarized the peer-reviewed data submitted to the FDA that justified its emergency use approval for the Pfizer vaccine. It looked pretty good to me too. I am trying to get the New England Journal of Medicine to allow me to reproduce the graph of the number and timing of new virus infections following administration of the vaccine or salt water. Those results blew me away. The short-term side effects were largely local, and in my mind acceptable. Hopefully the makers of the Moderna vaccine will present their data also– and may even have done so already. Therefore, I and public health experts are disappointed that so many healthcare workers, nursing home employees, teachers, and others are not electing to become immunized when it is made available to them. Those occupational locations are mixing bowls for the community spread of Covid-19 disease just as in restaurants, bars, movie theaters, churches, and other places where people gather together. The explosive rise of cases in Lee County where the state prison is the major employer is an example of how the virus leapfrogs around the community. In a county with a population of only 7403 in 2019, there were 1055 cases of Covid-19 reported!
Or not.
It appears to be a given in Kentucky that it is politically impossible to require immunization for employees or other individuals who are in positions where they can transmit disease to others. I propose that we may not be able to dodge bringing such a discussion out into the open. Surely there are precedents and limitations on the ability of an individual to hold out on public health obligations. When I was still practicing medicine, I and my colleagues had to submit to getting an annual chest x-ray to prove that I did not have tuberculosis in order to remain on hospital staffs. There would have been some small risk to us from the x-rays. Don’t some healthcare settings already require employees to get flu-shots? Infectious diseases used to be by far and away the most common cause of death. Child mortality was high, and lifespans were much shorter than today. Public health measures including immunizations were the literal lifesavers. Courts have upheld vaccine requirements for schools. (Do we not have such a requirement in Kentucky? Do we have a statewide registry? Why not?) What justifies a religious exception to refuse vaccination? The Constitution protects the ability of an individual to believe in whatever vision of God they choose or not to at all, but neither category of believer allows one to act in whatever way they wish in either the private or public arena. For example, it is an established principle that there are legal limits for parents to prevent their children from receiving effective life-saving medical treatment. Haven’t members of the armed forces been required to get their shots when they enroll? There are laws against child marriage and snake-handling by children. I have not even begun to assemble such a list. Naturally this is a sensitive and difficult public policy matter to consider. Opinions will be strongly held. Nonetheless, if we are not collectively able to bring the current pandemic under control, we may as a nation have to consider what the reciprocal obligations between citizen and the communities in which they live. How bad will we let it get before we do so?
Peter Hasselbacher, MD
Emeritus Professor of Medicine, UofL
Kentucky Health Policy Institute
24 January 2021
