I thought that before I signed the death certificate of the Posting Standard Charges Project, that I would place a mirror beneath its nostrils just to make sure it was ready to put in the ground. I was planning to add this confirmatory step as an addendum or comment to my first article, but it was clear that additional details and discussion would be necessary. My first pronouncement was based on a bedside-look at the several chargemaster databases. What did the local hospitals choose to disclose; what must they have intentionally omitted; how easy was it to find anything; and was the information useful to compare different hospitals? I did not even have to feel for a pulse to know the answers. Out of fairness and a desire not to bury the patient alive (but with certainty that my initial diagnosis was correct) I applied a more definitive diagnostic test that might been a valid real-world trial for me had these posted standard charges been available last Fall.
As I pulled away from my cardiac pit stop at Rhode Island Hospital, it was suggested I schedule a cardiac echo stress test back home to evaluate the size and function of my heart. Using all of my wisdom and experience as a physician and Professor, I did what everybody else does– find a cardiologist who would see me as a new patient and do what they suggest! The stress test was normal. I could not have hoped for a better result nor more competent and attentive care. The question for our present exercise is: If posted standard charges were available– and I had time to look at them– what I have found? [Spoiler alert! The effort would have been a waste of time, if not misleading.]
How would I know what to look for?
Since no search function is provided on their websites to access their standard charges by any of the hospitals, I had to structure my own searches within an Excel spreadsheet using a “filter” on the charge-description column to find any or all billable item descriptors containing the word “stress.” (If you do not understand what I mean by this, do not bother opening up the chargemaster files!) Even if the user is facile with Excel or other spreadsheets, this was not as straightforward as one might think. For example, the lists from Jewish and Sts. Mary contain atypical, non-printing characters that defied attempts to sort or seek. [I devised a multistep technical work-around that most real-world users would have trouble with!] After coming up empty with searches for ‘cardiac’, or ‘heart’, it turned out that the magic word was “stress.” (A user would need to know enough about medicine and medical billing to ignore the other kinds of stress tests that pop up with this search word.) I must confess that I am not at all confident that I found all the relevant items I would have needed. In my opinion, even a professional medical billing person would not find enough information in these chargemasters to predict how a patient’s final bill would be structured let alone what it would cost. Some research on my part was necessary to make more sense of things but the result was only additional layers of confusion.
What is a Cardiac Echo Stress Test?
Of course by now, I have already had one variety of the test. It involved showing up at a hospital outpatient office wearing athletic attire. I had a baseline (resting) cardiogram and cardiac echo which can show my heart and its valves in motion. The echo (ultrasound) was done through my chest wall. I was given an intravenous injection of a lipid -containing product (Definity) that shows up on the ultrasound (echo) outlining the heart chambers and enabling the operators to measure chamber size, motion, and the thickness of heart-muscle walls. With a multiplexity of wires still attached to my chest and an I.V. in my arm, I was then transferred to a treadmill on which the speed was progressively increased. The nurse/technicians continuously monitored my EKG to make sure there was no signs of ischemia (insufficient blood flow to the heart muscle itself). When I got to the maximum speed of the test and/or heart-rate for my age, I was quickly assisted back onto the examining table where another cardiogram, cardiac ultrasound, and injection of contrast material were performed. When I eventually saw the report, I was amazed at the amount of detail that can be captured. I could only think back to my training years when we had to guess whether a heart murmur was significant or not; or whether perceived chest pain was coming from the heart or elsewhere; and when we had little more than physical inspection of the chest wall, neck veins, or plain x-rays to estimate heart size and function. We’ve come a long way baby!
What to Search For?
To make any sense whatsoever out of the numbers provided by the hospitals I had to do some on-line research. Simply Googling “billing for cardiac ultrasound stress test” brought up an overwhelming amount of information– mostly confusing to me. Charges depend on whether or not the ultrasound is done through the chest wall or through the esophagus; whether or not the electrocardiogram monitoring is done continuously or only at both ends of the stress; whether or not the “stress” is administered by exercise or by a drug that stimulates the heart directly; whether or not contrast material is administered; what kind of contrast materials is used and whether or not it is billed separately; whether the test is done in a provider’s private office or in a hospital facility where it gets higher payments; for the creative billing talent of the provider; and perhaps other things not apparent to me. Different combinations of these factors determine what CPT billing code would be used (and paid for) by insurers. There would be additional charges facing a patient for the test including cost of the specific contrast agent used, physician fees, other x-rays and tests, and who knows what else!
Cardiac Echo Stress Tests in Louisville.
I include a list below a list of all of the descriptors I could find for the hospitals in this survey (and a PDF document with the data). I doubt I have found all the relevant items.
Selected Observations.
• None of the hospitals used the same words or abbreviations for the item descriptors. Even for identical descriptors there can be different prices for the same hospital!
• Lots of abbreviations will be confusing to many: TTE= Transthoracic Echo; US= Ultrasound; W= With; WO= Without; HC= I don’t know!; Dobutam= Dobutamine (a drug); ECG= Electrocardiogram; DOPPL= Doppler (a kind of echo). Although the prefix “cardio” appears in some of the descriptions, the word “heart”or “cardiac” is not used.
• Although Jewish Hospital and Sts. Mary & Elizabeth operate under the same Medicare provider number and are considered by Medicare as a single financial unit, it is apparent that from their charge masters that different descriptors and prices are used.
• Baptist no longer appears to have the lowest charges in town as it did in the 1990s, at least for this service.
How much will the study cost? [Spoiler alert: There is no way to tell.]
If we use the listed charge as a possible general indicator of how high a given hospital is bold enough to charge, then there are major differences between our local and university hospitals. Only the two University Hospitals posted charges for at least one version of the test that exceed $4000. (These are the hospitals in this group whose patients have the least ability to pay!) Baptist was not far behind with charges that mostly exceeded $3000. At the lowest end of the standard charges was Clark Memorial at $1684. Jewish and Sts. Mary & Eliz were somewhere in between. I could not find an entry for Norton Healthcare using their chosen presentation format- and I tried!
Does that mean that folks with an option should go to Clark Memorial, or for that matter to avoid the University Hospitals or Baptist? Not necessarily. One issue is that there will undoubtedly be associated charges with the basic stress test procedure. These will include physician and operator fees, charges for drugs and intravenous administrations, and other add-ons that can be significant. I suspect these things are unknowable in advance to mortal beings. They were to me. The final charge will almost certainly be higher, perhaps considerably so as mine was. It is important to consider that there are no indicators in these tables of the quality of the services offered or the experience of the providers with the service. Nor is there any reason to assume that the more expensive, the better the quality or outcome.
Who pays what?
The real problem with these chargemaster lists of standard charges is that for the majority of people being studied, the actual amount a patient will be responsible for is lower, in fact for people with most kinds of health insurance– much lower! For example, the bill sent by a hospital for my outpatient facility study to Medicare was for $6168. Medicare’s contracts with participating providers and hospitals discount any charge, no matter how high, to an total of $449 which Medicare and my Medicare Supplement policy split 80:20. (Of course I had to pay the premiums for Medicare and a Medicare Supplement which I am fortunate enough to be able to afford.)
Medicare not the only third-party payer that sets prices.
Virtually every other health insurance entity has similar contract prices with health professionals and hospitals in their networks. To some degree or another, our survey hospitals point out somewhere in their webpages that they are required to have policies in place for charity care or reduced charges for the medically indigent. One danger of making the chargemaster lists available is that fear of wallet-damage or bankruptcy will cause someone who needs a test not to get it! In my opinion, UofL Hospital does the best job in trying not to scare prospective patients away- kudos! Right at the top within the Chargemaster Database itself is the following statement:
“University Medical Center has made public the charges for all elements of patient care. These rates do not include professional/physician fees such as pharmacy, diagnostic imaging, or lab work. “The hospital’s charges are the same for all patients, but a patient’s responsibility may vary, depending on payment rates negotiated with individual health insurers. If you have questions about your financial responsibility, please contact your insurer. Uninsured or underinsured patients should contact our financial counselors at502-*****) to determine if they qualify for discounts. Emergency services will never be delayed or withheld on the basis of a patient’s ability to pay. These prices are correct as of January 1, 2019.”
I could not have summarized better myself why the mandatory posting of standard charges by the current federal administration makes no sense at all if its purpose if to allow citizens to make intelligent decisions about their health care. The obvious follow-up question I have is why do we allow such an obviously insane system to exist? If it has any benefit, what is it and for whom? Is it really true or is it a lie that no one is billed for, or pays full charges? ‘Standard Charge’ is an oxymoron, or at least a gross distortion of the English language. Perhaps ‘standard gouge’ would be more accurate.
Bottom line for Hospitals?
So what do hospital’s outpatient centers and doctor’s offices actually get paid for a basic Cardiac Stress Echo. I have no way to know for sure, but here is at least one approach to an estimate. [Any providers out there want to give us some figures for different insurers?]
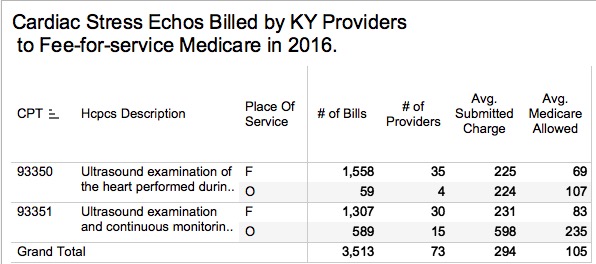
Medicare provides a public-use-file yearly for payments to physicians and other providers in the fee-for-service portion of Medicare. Every individual service performed by a given named provider more than 10 times is itemized, including number of times billed, total charge submitted, and the amount allowed by Medicare. In 2016 Kentucky, Medicare was billed by physicians for 3,513 cardiac stress echo tests. These were split about evenly between CPT code 93350 and 93351– the latter including continuous monitoring and which pays a little more. There were only about 40 individual providers listed for each code with some providers who used both codes counted twice. If the test was done in a facility other than the doctor’s office, the average charges submitted to Medicare were $225 and $231 for the two codes respectively. However, Medicare allowed payments of only $69 and $83! If the procedure was performed in the providers private office using their own equipment, and not in a hospital or other outpatient facility, the average charges were $224 and $598, and the average allowed payments $107 and $235. It is well known and controversial that Medicare pays more to hospital’s off-campus outpatient clinics for the same procedure than if it done in a private doctor’s office. Thus, we can assume that Medicare pays a hospital more than $235 for a cardiac echo stress test, but how much more is not known to me.
Where should I go?
Is this an argument to try to get tested in a private office (O)? I cannot say. There is still a wide range in charges submitted to Medicare by individual physicians for this service. I do not know if the facilities (F) appearing in the 2016 stress test numbers use the same Chargemaster when it submits its bills to Medicare. Perhaps a Medicare bill from a facility uses different chargemaster amounts. What can be gleaned from these individual provider reports is that physicians ordering or doing the tests in either their offices or a facility are accustomed to receiving only a small portion of what they charge. Medicare protected my pocketbook (and heart) but might not yours if you have another health insurance payer or none at all. [Is a Medicare option for all looking better to you now?]
I have probably numbed-out your minds with all this detail. It took me a couple of days to organize things even this far but I still have had nothing better to go on should I need to have this procedure again. I conclude that the mandatory posting of standard charges would not even allow a professional medical coder to be able to predict a patient’s bill from the data presented. I am now confident enough to tie a tag on the toe of the chargemaster system as having no utility to a patient and to start shoveling in the dirt. All this was no secret to the US Department of Health and Human Services or its Health Care Financing Administration, nor to hospitals themselves which argued strenuously against the mandate. One can only speculate why this small part of Obamacared was pushed forward at this time. As far as I am concerned, the only value to the initiative is to embarrass hospitals for billing outlandish charges to those least able to pay, and to shame the rest of us for allowing it to happen.
Peter Hasselbacher, MD
Emeritus Professor of Medicine, UofL
President, KHPI
January 29, 2019