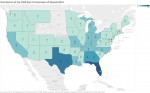
FDA and Medicare Records reveal Sackler-Associated Drug Companies as Leaders in Controlled Substance Markets.
In the Pre-Covid Era, almost every day’s newspaper would contain at least one article about our last-worst epidemic of opioid abuse. Since Covid-19 justifiably soaks up much of our attention, the infrequent article about opioids now takes me by surprise. The odd article that leaks through reminds us that the opioid tragedy has not gone away. Indeed, as the desperation attendant to Coronavirus spreads, there is every reason to believe that the fellow-traveler of opioid abuse is blossoming also. The current news environment has allowed the progress of previously reported high-profile litigation against an assortment of opioid manufactures, marketers, and sellers to proceed in the relative background.
Last week, the United States Department of Justice announced that one arm of litigation came to a head when Purdue Pharma LP pled guilty to three felony charges related to its marketing and distributing of OxyContin. The settlement agreement (subject to bankruptcy court approval) includes a payment of $8.34 Billion, but to whom or what is not clear to me. Since Purdue declared bankruptcy, it seems unlikely that anywhere near that amount will ever be paid. Companies don’t go to jail. Even billions of dollars can be an tolerable cost of doing business in Big Pharma. As part of a broader overall settlement, the Sackler family owners of Purdue resolved a number of additional civil charges for $225 Million. Some commenters have expressed opinions that the Sacklers and Purdue are getting off easy. That may well be so, but the Justice Department’s announcement notes that “the resolutions do not include the criminal release of any individuals, including members of the Sackler family, nor are any of the company’s executives or employees receiving civil releases.” In my opinion that is eminently proper.
Continue reading “Proposed Purdue Pharma DOJ Settlement Emphasizes Role in Opioid Epidemic.”